The children malaria is taking in Lango
Doctors explain that in severe cases, malaria parasites can damage red blood cells and block small blood vessels, reducing oxygen supply to critical organs.
An Anopheles mosquito in the lab_Target Malaria. (Credit: Hudson Apunyo)
_______________
A storm gathers as we take the turn off Apac road to Teoryiang village, Nambieso sub-county in Kwania.
It is dusk. Lightning flickers ahead, illuminating the rough road in flashes. It is raining where we are headed.
In the vehicle with us is 27-year-old Kela Obura, who has just buried a child she lost to malaria.
As we navigate through the bushy and dark road, her mood changes. She grows quiet, lost in memory.
Soon, she is moved to tears.
Malaria pain
Obura’s voice trembles as she points to the final turn to her father’s home, where her son, Kicarwot Timothy, was laid to rest.
The journey from Lira city has taken two hours.
Dr Jimmy Alaal, a medical officer in pediatrics at Lira Regional Referral Hospital, has come with us. He helps translate our conversation, his voice empathetic.
It is all emotional.
Emotional moment: Kela Obura sheds tears as she narrates what happened to her son. (Credit: Hudson Apunyo)
Obura narrates how it all started for her firstborn. He had been weak, feverish, and hadn’t been eating for a day, right here where they lived along the shores of Lake Kwania.
She struggled to find sh15,000 the following day to reach Nambieso Health centre III. Kicarwot was diagnosed with malaria, but his condition worsened within two days.
They were then referred to Aduku Health Centre IV, which required sh25,000 for a boda boda. Without a job and her father, Henry Okonye, a subsistence farmer, they had to borrow the money.
By then, “the child was vomiting out everything he swallowed, his temperature remained high, and he had developed breathing challenges”. The healthcare centre could not handle the complicated case of malaria, so Kicarwot was referred to Lira Regional Referral Hospital in Lira city.
There, Dr Alaal and the team took over the case, administered the required treatment, but due to the severity and other complications that had developed, he didn’t make it.
On March 24, 2026, four-year-old Kicarwot Timothy was pronounced dead.

Obura and her father pay respect to her son. (Credit: Hudson Apunyo)
Kicarwot’s story is not isolated. Many families in Lango are facing the same threat, and some are already in the fight to survive malaria.
Hospital battleground
At the Lira Regional Referral Hospital, cries of babies and young children are deafening.
It is 1:00pm, and the number of patients - mostly mothers carrying sick children - keeps soaring as records are taken at the acute unit of the outpatient department.
Robson Okabo, the principal medical clinical officer, says “the pressure is overwhelming and the numbers can go to 1,500 on some days”.
The sitting area is full. Some people are standing. Some are leaning against the wall. There is a mother breastfeeding seemingly weak twins, one on each side, as she waits her turn.
Patient names are called over the loudspeaker, directing them from one stage to the next - records, triage, the clinic and laboratory, and finally, treatment is administered.
Okabo says, “No patient dies at the outpatient department”. Those who come in in severe condition are rushed to the emergency and admitted.
But not all cases arrive in time.
Some, like Kicarwot Timothy, reach here when the illness has advanced.
Most of the children arriving at Lira Regional Referral Hospital are battling severe malaria.
The facility recorded 2437 malaria cases at OPD between October and December 2025.
“It is a heavy burden for the Lango region because of the vegetation and climate,” Dr Andrew Odur, director, Lira Regional Referral Hospital, explains, adding that, “malaria is still among the top five causes of morbidity and mortality within the hospital”.
Inside the body
When malaria doesn’t take a life, it takes the quality of life.
By the time many patients are diagnosed with malaria, they have already developed complications.
Doctors explain that in severe cases, malaria parasites can damage red blood cells and block small blood vessels, reducing oxygen supply to critical organs.
The kidneys, brain, and lungs are among the most affected, leading to complications such as acute kidney injury (AKI), cerebral malaria, and breathing difficulties.
A review of malaria-associated acute kidney injury in African children published in the International Journal of Nephrology and Renovascular Disease found that 24% to 59% of children with severe malaria develop AKI.
Five-year-old Marceline Ayongi from Lira hadn’t passed urine for a week, and her condition required dialysis to stay alive.
Her mother, Rebecca Adimo, didn’t have the money for dialysis, so she was referred to St. Mary’s Hospital, Lacor, for the cheaper peritoneal dialysis in which locally mixed fluids are used. She confidently says, “I’m not scared now, my girl has fully recovered”.
A recent JAMA study conducted in Uganda has linked childhood cerebral malaria and severe malarial anemia to “cognitive impairment and decreased academic achievement later in life”.
Dr Daniel Ogwal, a medical officer at Lira Regional Referral Hospital, is among the team studying “malaria-associated pathogenesis of chronic kidney disease” in Mulago, Jinja and Lira, following children who had severe malaria and following them over a two-year period to see how many develop chronic kidney disease and comparing them to children who didn’t have malaria.
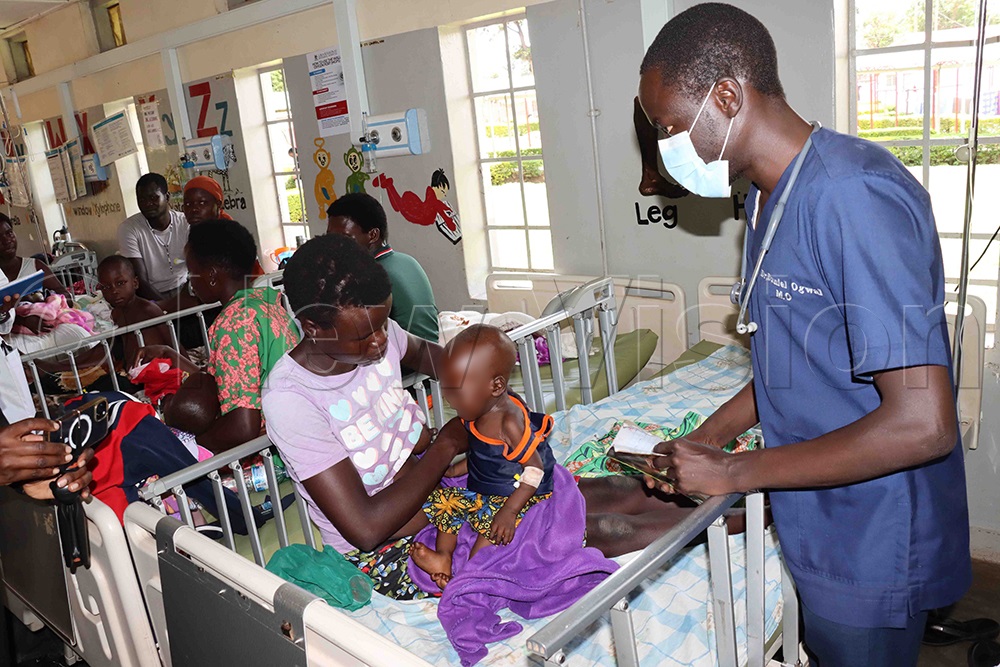
Dr Daniel Ogwal, a medical officer at Lira Regional Referral Hospital. (Credit: Hudson Apunyo)
In the past one year, “we have had about 7,500 malaria cases… some are treated under outpatient, and others are admitted and treated for severe malaria… Some of these children die before reaching the hospital”, Dr Ogwal says.
At the Lira site, 26 of the 200 patients sampled died of malaria.
“We would have hoped that by now we would have a significant reduction, but because of our environment, the mosquitoes breed, grow, and there are many,” Dr Odur says.
Government response
Despite understanding what malaria does inside the body, preventing severe cases remains a challenge.
Dr Alaal came in handy when our car battery died.
It was way past 9:00pm, and we needed to get out of Nambieso, where we had gone to see Kicarwot Timothy’s burial site and meet the grieving family.
The rest of us were frightened, but he confidently rode a bicycle to go find a battery, and he did before we successfully jump-started the car.
He told us that he “used to do a lot of field work before becoming a medical officer” and that he had “experienced worse scenarios during community outreaches.”
The government has undertaken ambitious campaigns in the fight against malaria. All require reaching out to communities.
The Malaria Elimination Strategy 2025–2030 aims for at least 80% coverage of preventive interventions.
It includes the ongoing distribution of 25.8 million long-lasting insecticide-treated nets across 130 districts, focusing initially on northern and eastern regions.
The 24.2 Hours Initiative aims to ensure that anyone showing symptoms of malaria is tested and treated within just 24 hours, and within two hours of reaching a clinic.
“Whoever is identified to have severe disease and they require care within two hours, they are able to receive it within the stipulated two hours,” says Dr Jane Irene Nabakooza, the technical lead, malaria prevention and vaccine, Ministry of Health.
Between 2009 and 2018/19, the country reduced malaria prevalence among children under five from 42% to 9%, progress driven also by residual spraying.
But new data from the 2024–25 Malaria Indicator Survey by Uganda Bureau of Statistics shows a reversal; prevalence has risen to 21%. In some regions, the situation is even more severe, reaching 59% in Lango, 46% in Acholi, and 44% in Teso.
Gene drive
Even with existing interventions, malaria continues to persist, pushing researchers to explore new tools.
“Most people fear that if we bring in novel genetic control tools, they are going to wipe out all mosquitoes, no. It is only those few species that have the capability to bite you and transmit malaria to you, to your mom, to the little girl who is sleeping or to the baby,” Dr Martin Lukindu, researcher, Target Malaria explains.
Target Malaria is one of the research projects developing gene drive mosquitoes. Part of a consortium of research institutions in Africa, Europe and North America, Target Malaria researchers and scientists are working to reduce the population of malaria mosquitoes, because fewer mosquitoes carrying malaria would mean stopping the transmission of the disease.
It is a bold new tool, the ministry of health is evaluating, as Dr Nabakooza explains.
“For the national malaria elimination division to consider any technology, we usually conduct research to make sure that it is feasible, it is acceptable, it is cost-effective, and it will work in our kind of context.”
Gene drive mosquitoes are being researched in controlled laboratory settings. “For now, I wouldn’t be firm to say that we are considering what we are doing, as ministry of health is to evaluate the mosquito gene drive technology. If we get positive results, then we shall consider it for our national strategic plan.”
There are two gene drive strategies currently under investigation among various research teams in the world: either to reduce the number of malaria-carrying mosquitoes or to stop the parasite from infecting the mosquitoes.
The focus in Uganda is on reducing mosquito populations.
“It is important to note that we do not target all mosquito species, but focus on the main malaria-transmitting Anopheles species,” Dr Jonathan Kayondo, principal investigator, Uganda Virus Research Institute.
He defines gene drive as “a naturally occurring biological process that is being harnessed into the technology. In living organisms, gene drive increases the chance of inheritance of certain genes or traits”. Gene drive is being researched to be a complementary tool to fight malaria in Africa, working alongside bed nets, insecticides, drugs and vaccines.
“By biasing the rate of inheritance of certain genes from one generation to another, gene drive can spread a modification to be passed on to the entire mosquito population,” Dr Kayondo explains.
There are currently no gene drive mosquitoes in a contained laboratory in Uganda; they have so far never been released in the wild.
Target Malaria hopes to conduct gene drive field trials by 2030 in a malaria-endemic African country like Uganda.
And until that moment comes, Teoryiang villagers remain wary of mosquito bites.
Kicarwot’s grandfather showed five nets, which became dirty after use during the burial.
Tucking them away, they joked that because of its beauty, Nambieso was the chosen area for the development of a town, but too many mosquitoes forced the move to where Lira is today.
Anopheles gambiae is one of the main mosquito species responsible for transmitting malaria in Uganda, and it commonly carries Plasmodium falciparum, the parasite that causes severe malaria in humans.
Apac burden
While new technologies are still years away, the burden today is most visible in districts like Apac.
The image of Obura and her father dusting the epitaph on her son’s grave at 9:00pm is lasting.
To think mosquitoes that sting us every day transmit a disease so deadly that it is the number one killer of children in Uganda is confusing.
They are just mosquitoes.
But deadly vectors.
Apac and the wider Lango sub-region experience some of the highest malaria transmission and mosquito exposure levels in Uganda.
It is the epicentre of malaria in Lango and in Uganda, “well known worldwide for malaria burden”, Dr James Daniel Odongo, the district health officer, says.
The district continues to record high transmission rates, with children under five bearing the greatest impact.
In the 2024/25 financial year, Apac recorded 3,441 malaria cases among children under five. In 2025/26, the number reduced to 1,803 cases.
He says the decline reflects ongoing prevention efforts, but cautions that malaria remains entrenched in the community.
Apac has also scaled up prevention measures, including malaria vaccination, which the ministry of health rolled out last year. Health records show that 2,255 children have received the malaria vaccine, with coverage estimated at about 79 per cent.
“We registered a reduction in mortality among children below five years by half between 2025 and 2026, but we would wish to have zero deaths due to malaria across the district and across age groups.”
Ahead of World Malaria Day on April 25, the World Health Organisation prequalified for the first time malaria treatment for babies, an artemether-lumefantrine formulation for infants weighing 2–5kg, raising hopes of further reducing deaths in hard-hit regions like Lango.
But for some families, that progress is still a far cry from their reality.
In Teoryiang, Nambieso, Kela Obura still visits a small grave on the side of her father’s compound.
This reporting was produced with support from Target Malaria.